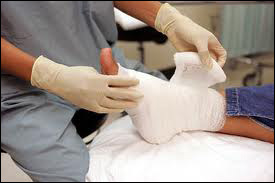
 Diabetes and wound care has grown to be a critical subject over the years. Approximately 5 million Americans suffer from some sort of chronic wound or open sore, 15% of these are diabetics. Chronic wounds can become infected, develop gangrene or require amputation. Diabetics are at a greater risk of developing chronic wounds because of poor circulation, slow healing times, vascular disease and neuropathy (numbness). Diabetic ulcers is a leading cause of lower extremity amputation.
Diabetes and wound care has grown to be a critical subject over the years. Approximately 5 million Americans suffer from some sort of chronic wound or open sore, 15% of these are diabetics. Chronic wounds can become infected, develop gangrene or require amputation. Diabetics are at a greater risk of developing chronic wounds because of poor circulation, slow healing times, vascular disease and neuropathy (numbness). Diabetic ulcers is a leading cause of lower extremity amputation.
Because of this fact we will focus on diabetic foot ulcers, the most common of all diabetic chronic wounds. We’ll discuss how ulcers form, what treatments are available to you and how to prevent ulcers. Patient education regarding foot hygiene, nail care and proper footwear is crucial. Let’s get started.
What is a Foot Ulcer?
Foot ulcers are open wounds that develop on the sides, top or soles of the feet. Diabetics are prone to these wounds because of poor circulation and other problems that arise from having diabetes. Diabetes and wound care should be taken seriously. Diabetic ulcers are notoriously difficult to treat and the treatment can be lengthy and frustrating. Lower extremity morbidity, particularly foot wounds account for one quarter of all diabetic hospital admissions in the U.S. and Great Britain.
Who Gets a Diabetic Foot Ulcer?
Almost anyone who has diabetes can develop foot ulcers.
Who is more likely to develop foot ulcers?
Statistically it’s African Americans, Native Americans, Hispanics and older men.
Who is at risk?
People who use insulin and those who suffer diabetes related ailments such as heart disease, kidney and eye problems are equally at risk. If you are overweight, smoke and use alcohol you are at a greater risk of developing foot ulcers.
How Do Diabetic Foot Ulcers Form?
There are 4 major causes of diabetic foot ulcers.
Neuropathy (numbness).
Neuropathy is a condition where you lose sensation in your limbs and lower extremities. Prolonged elevated glucose levels over time cause this to happen. This condition has a way of creeping up on you. Often you are not aware of the problem until it’s too late. Because of numbness patients can’t feel small cuts on their feet, wounds can go untreated for days even weeks. Also neuropathy can cause a patient not to shift or move their feet when pressure points develop. This can lead to wounds developing. Your doctor can check your feet using a simple painless test with a tool called a monofilament.
Foot deformities.
Because of neuropathy patients can break bones in their feet and not be aware of it. Foot deformities can put unnatural pressure on certain areas of the foot and cause wounds to develop.
Vascular Disease.
This disease causes narrowing of blood vessels and can lead to wound development. Restricted blood flow and circulation make treating foot ulcers frustrating and lengthy. This condition reduces the body’s ability to heal itself–which increases the risk of infection.
Skin irritation and friction.
Patients with neuropathy (numbness) cannot tell when they have skin irritation, problems with friction or pressure points. The only way to know for sure is to check your feet often for redness, peeling skin or blisters.
How Should a Diabetic Foot Ulcer be treated?
Prevention, prevention, prevention. Diabetes and wound care is all about prevention. You know what they say about an ounce of prevention. Untreated wounds can lead to infection. The quicker you treat the wound the less likely you are to develop a problem.
There are 3 commonly used treatments for foot ulcers.
Offloading – That’s offloading off-roading. It means quite literarily putting your feet up. Reducing pressure on a wound is probably the single most important and most neglected factor in chronic wound treatment. It could mean anything from using crutches or a wheelchair to complete bed rest. Taking a load off sounds like a nice idea but it could take anywhere from 6-12 weeks for your wound to properly heal. That’s a lot of downtime.
This is where doctors have a problem. Their patients rarely ever follow the proper protocol. So, listen to your doctor!
It’s a little technical, written for doctors by doctors but it’s very informative.
Debridement – The removal of dead skin and tissue. Dead tissue can slow or impede the healing process. The dead skin can appear yellow, tan or black in color. A doctor usually includes debridement as part of complete diabetes wound care protocol. There are 4 ways to debride a wound, autolytic, mechanical, enzymatic, and surgical.
Applying medication or dressings – This is usually used in conjunction with other treatments. Your doctor will advise you what medication or dressings to apply. In most cases you will be responsible for changing the dressing and keeping an eye on the wound. The medication could be a course of antibiotics or simply an antibiotic ointment. With diabetes, wound care can be a big responsibility for the patient.
How to Keep a Foot Ulcer from Becoming Infected. If you want to keep a foot ulcer from becoming infected, there are a few things you need to do.
Control your blood sugar levels – It is vitally important that you control your blood sugar level. It’s especially important during the time you are receiving treatment for diabetic foot ulcers. Try to avoid and reduce the risk of infection while undergoing treatment–consult your doctor about the steps you should take to control your blood sugar. Eat right, exercise and check your levels daily.
Keep the wound clean and bandaged – The old way of thinking about wounds, “let it breathe”, is not correct it can impede the healing process. Keep a wound clean, covered and moist is the way to go. Clean the wound daily. Cover it with a medical bandage. Keep the wound or ulcer moist–with creams or antibiotic ointments. Not moist as in; whirlpools, peroxide, soaking or full strength Betadine. These things are not recommended for healing a wound or ulcer. They can in fact make things worse.
Do not walk barefoot – Diabetics often suffer from neuropathy (numbness). As a result, they won’t feel it if they accidentally step on a tack or a piece of glass. The subsequent wound could be difficult to heal, or worse, become infected and lead to serious consequences. So, keep your feet covered.
Never reuse a syringe – As a rule our skin acts as a good barrier to most infections. But if you are on insulin, you routinely have to breach the surface of the skin and puncture the underlying tissue. From the minute you uncap the syringe it is exposed to the atmosphere of the room. After drawing in the insulin, the needle is moist. So you are administering a shot with a moist needle exposed to the room temperature and atmosphere. It would be unwise to recap a moist syringe after puncturing the skin. Make sure you always have a healthy supply of syringes on hand and that you never run out.
How Can a Foot Ulcer be prevented?
The best and by far the easiest way to prevent a foot ulcer is…. never getting a foot ulcer! Other than the obvious, you can follow the steps recommended above. Wear shoes; keep your feet covered with heavy or thick socks. They should fit snuggly but not too tight, you should avoid constriction. Every time you buy shoes you should have your foot measured and sized correctly. Clean and inspect your feet daily. Try to correct any foot deformities such as bunions, corns or hammertoes.
Take care to reduce all risk factors such as; drinking alcohol, smoking tobacco and uncontrolled blood sugar levels.
Self-Care Products and Diabetic Wounds
There are many products available on the market today, so called “beauty aids” for the feet. It can be a treat on occasion to have a home pedicure. However, if you are a diabetic these products can lead to open wounds.
For example, there is the “pumice stone”, a hard abrasive stone used to scrape away “dead” skin from the foot. If you’re a diabetic this can leave cuts and abrasions on your feet that won’t heal. There is something called a “corn plane”, this device operates exactly like a wood plane. Instead of shaving away wood pieces, you are shaving away skin. In the category of corn and callus removal, there is salicylic acid. The way this acid works is to slowly erode skin that makes up warts, corn and calluses.
The most common of these self-care products is the nail clipper. Most people cut their nails too close to the cuticle. If you are diabetic you should see a podiatrist regularly and let your doctor advise you on the best way to care for your feet.
